What Does It Mean to Heal Trauma? A Survivor-Practitioner's Perspective
Malachi Gillihan is a Trauma Specialist in Berkeley, California who works with survivors through individual sessions, groups, workshops, and retreats, both in person and virtually. This piece is his working answer to a question every survivor eventually asks, and one many practitioners fumble: what does it mean to heal trauma, really? After more than three decades of living with the symptoms of post-traumatic stress and more than twenty years of studying, training, and walking alongside other survivors, he offers not a final definition but a clear, honest map.
If you have been asking this question yourself, you are already doing the work. Book a free consultation when you are ready to talk about what healing could look like for you specifically.
Why This Question Is Harder Than It Looks
Here is something I noticed after years of working with trauma, first as a client and then as a practitioner: when two people say the word "healing," they are almost never talking about the same thing.
A survivor might mean, "I want to stop having flashbacks." A practitioner might mean, "I want to help you widen your window of tolerance so the flashbacks lose their grip on your life." A researcher might mean something else entirely. None of these are wrong. But if nobody says out loud what they actually mean, expectations collide in quiet, discouraging ways. A survivor can walk away from real, significant healing work convinced that nothing happened, because what they were privately hoping for was something nobody ever promised them.
So before I offer my own working definition, I want to name that gap. The word "healing" is carrying a lot of weight. Different sources, the DSM, medical textbooks, research journals, Eastern contemplative traditions, Western somatic practitioners, will all give you different answers. That is not a bug of the field. It is just the territory. Judith Herman's Trauma and Recovery (2015) gave the field one of its most durable frameworks, three stages of recovery (safety, remembrance and mourning, reconnection), and even that deeply useful model is not meant as a universal definition of what healing is. It is one careful articulation among many.
My own version of this question became impossible to ignore after I was formally diagnosed with PTSD in 2018, more than three decades after the child sexual trauma I experienced at age eight. For most of those three decades, no one in my care used the word trauma. I collected other diagnoses instead, each one tackled independently, compartmentally. The best any of them could offer was symptom management. Recovery was not discussed as a possibility.
When I finally began body-based trauma work, something unexpected happened. The work did not just reduce symptoms. It produced profound shifts I can only describe as spiritual. Around the same time, I read Peter Levine's Waking the Tiger and found his now-famous line: "Trauma has the potential to be one of the most significant forces for psychological, social, and spiritual awakening and evolution" (Levine & Frederick, 1997). Here was a pioneer in the Western trauma field saying, in print, what my own body had just taught me. That was the moment the question became the center of my academic and clinical life.
The Scale of the Problem
Before the prevalence data, a brief detour. Human beings have been naming the territory of suffering for a very long time. The ancient Samkhya Karika opens with the line, "Because of the torment of the threefold suffering, there arises the desire to know the means of counteracting it" (Larson, 1969). The Buddha, centuries earlier, offered his first noble truth: dukkha, the recognition that life contains suffering. None of this is focused specifically on trauma. It describes the baseline difficulty of being human. Trauma layers on top of that baseline and makes the already-difficult significantly harder.
What makes this a pressing inquiry now, beyond the ancient backdrop, is scale. The estimates are staggering.
Research suggests that nearly half of all children experience some form of sexual violation before age 18 (Levine & Kline, 2008). More than half of all women experience some form of sexual trauma by adulthood (Miller, 1997). Bessel van der Kolk has argued that, within the United States, the abuse of children is the primary public health issue that needs to be addressed (Van der Kolk, 2015). These figures do not include sexual trauma in adulthood, date rape, domestic partner violence, workplace harassment, or any of the other categories that push the global total past one billion people.
Add other forms of trauma and the number climbs further still.
Here is the uncomfortable truth beneath those numbers: the way Western psychology has historically approached trauma has not been enough. The revolution sparked by body-based approaches, the work of Stephen Porges, Peter Levine, Bessel van der Kolk, Dan Siegel, and others, has forced a paradigm shift. And yet many of the institutions training today's practitioners are still catching up. Survivors deserve approaches that respect and value the body, because trauma lives in the body, and because trauma, especially sexual trauma, is often experienced as a potentially annihilating event. Talk alone cannot dissolve what the nervous system is still bracing against.
This is the backdrop. Now the question: inside this scale, inside this gap between how we were trained and what survivors actually need, what does healing trauma mean?
The Three Truths of Healing Trauma
After years of my own healing work, academic research, training under mentors including Dan Siegel and Deb Dana, and facilitating groups for other survivors, I have come to articulate what I call the Three Truths of Healing Trauma. They are not original discoveries. They are, I think, what every survivor is quietly waiting for someone to say out loud.
Truth 1: You Are Not Alone
One of the hallmarks of trauma is the felt sense of profound isolation. You are certain, in a bone-deep way, that no one else has felt what you have felt. That your experience is unique, unspeakable, and fundamentally private.
It is not.
I have sat in rooms with survivors who believed, before the room existed, that they were the only person on earth carrying their particular weight. Then they looked around and saw the weight on other faces. Something shifts in a nervous system at that moment that a thousand hours of solitary reading cannot produce. This is why group work is so central to my practice and toThe Octave, the group-based approach I developed during my master's work and piloted in 2022 with men who had histories of sexual trauma. The unintended finding from that pilot was unanimous and immediate: simply being in a room with other men who shared the experience was itself healing, before any technique was applied.
You are not alone. This is true even when your body is still insisting otherwise.
Truth 2: You Are Not Broken
The second hallmark of trauma is the conviction that you are, at your core, defective. That something about you is irreparably wrong. That whatever you are now is what you will always be.
This too is false, and the science now supports saying so clearly.
Human nervous systems have a natural push toward integration and health. Dan Siegel, one of the architects of Interpersonal Neurobiology, puts it this way: just as bones and skin know how to mend when broken, minds and nervous systems have an innate drive toward wholeness (Siegel, 2018). Trauma does not erase that drive. It impedes it. The mechanism is still intact underneath, which is precisely why healing work can reach it.
What feels like brokenness is, almost always, a nervous system that has adapted brilliantly to impossible conditions and is now waiting to be shown that the conditions have changed.
Truth 3: You Can Heal, and You Can Grow
The third hallmark is the belief that healing is impossible for you. Possible for others, maybe. Not for you.
I want to name something here. I am not promising a finish line. I am not promising the elimination of every difficult feeling you have ever had. I am saying that change is possible, that the change can be substantial, and that the change often includes growth that survivors did not believe available to them before they started. Levine's phrase, "trauma resolved is a gift of the gods" (Levine & Frederick, 1997), captures something I have watched happen in real rooms with real people. Not because a technique was applied, but because the nervous system, given enough safety and enough support, found its way back to its own natural intelligence.
This is also where my East-West training shapes how I hold the work. Contemplative traditions have long understood that suffering, met with the right conditions, can become material for transformation. Sri Aurobindo framed spiritual development as an integrative process rather than a shedding of the body and its feelings (Aurobindo, 1990). Debashish Banerji, writing in the same lineage, has articulated how becoming is not a linear climb but an ongoing unfolding that includes our wounds rather than transcending them (Banerji, 2016). I reference these not to impose a spiritual framework on anyone's healing, but because they describe the arc I have seen survivors walk when the work goes well, and they fit with what the science below says about integration.
These three truths are the spine of the work. Everything else, every framework I will walk through next, is scaffolding that helps us understand why they are true.
The Science That Makes the Three Truths Possible
If the Three Truths are the heart of healing, the theoretical frameworks below are the architecture. You do not need to memorize them to heal. But understanding them, even at a high level, can make the healing process feel less mystifying and more navigable. These are the lenses I rely on in my own practice and research.
Homeostatic Theory: Your Body Is Built for Flourishing
Neuroscientist Antonio Damasio offers a concept he calls the homeostatic imperative: a fundamental, built-in drive to not just survive, but to flourish (Damasio, 2019). This matters for trauma work because it upends a common misconception. Homeostasis is not boring, static balance. Damasio defines it as the continuous striving for what he calls "viable, upregulated life states that tend to produce flourishing."
Your feelings are the sentinels of this process. They are not obstacles. They are the signals your body uses to steer you toward survival and well-being. Trauma disrupts this signal system. It does not destroy it. Healing, in this frame, is the gradual restoration of the body's ability to feel its way forward.
Polyvagal Theory: Safety Is a Biological State, Not a Feeling You Think Yourself Into
Stephen Porges's Polyvagal Theory is probably the single most clinically useful framework I rely on. Three ideas sit at its core.
Neuroception is your nervous system's continuous, background scan of your environment for cues of safety or threat. This happens below conscious awareness. You cannot talk it into a different answer.
Three predictable response pathways. When your system reads safety, you are in a ventral vagal state: open, connected, curious, able to rest, digest, and relate. When it reads threat, it mobilizes you for fight or flight through sympathetic activation. If mobilization fails to create safety, the system drops into dorsal vagal shutdown: numbness, fog, collapse, dissociation. None of these are character flaws. They are biology doing exactly what it was designed to do.
Co-regulation is self-regulation. Porges's most quietly radical claim, and one Bonnie Badenoch has developed further in her clinical work (Badenoch, 2018): we cannot fully regulate our nervous systems on our own. We need the presence of other regulated nervous systems to do it. This is why connection is not a bonus feature of healing. It is the mechanism.
Attachment Theory: Earned Security Is Real
The work of John Bowlby, Mary Ainsworth, and more recently Allan Schore established that our earliest relationships shape our nervous systems in ways that predict long arcs of later health. If your early attachment was insecure, whether anxious, avoidant, or disorganized, that pattern often persists into adulthood.
Here is the part that matters most for trauma healing: it can change.
Through meaningful adult relationships, including the therapeutic relationship, many survivors develop what researchers call earned secure attachment. The old pattern does not get deleted. A new pattern gets built on top of it, strong enough to carry the weight of adult life. This is another way of stating what Polyvagal Theory already told us: we are hurt in relationship, and we are healed in relationship.
Interpersonal Neurobiology: Integration, Not Erasure
Dan Siegel's framework of Interpersonal Neurobiology (IPNB) rests on a single central idea: health equals integration. Integration is not the blending of everything into sameness. Siegel's phrase is "a salad, not a smoothie." It means differentiated parts remaining in healthy relationship with each other.
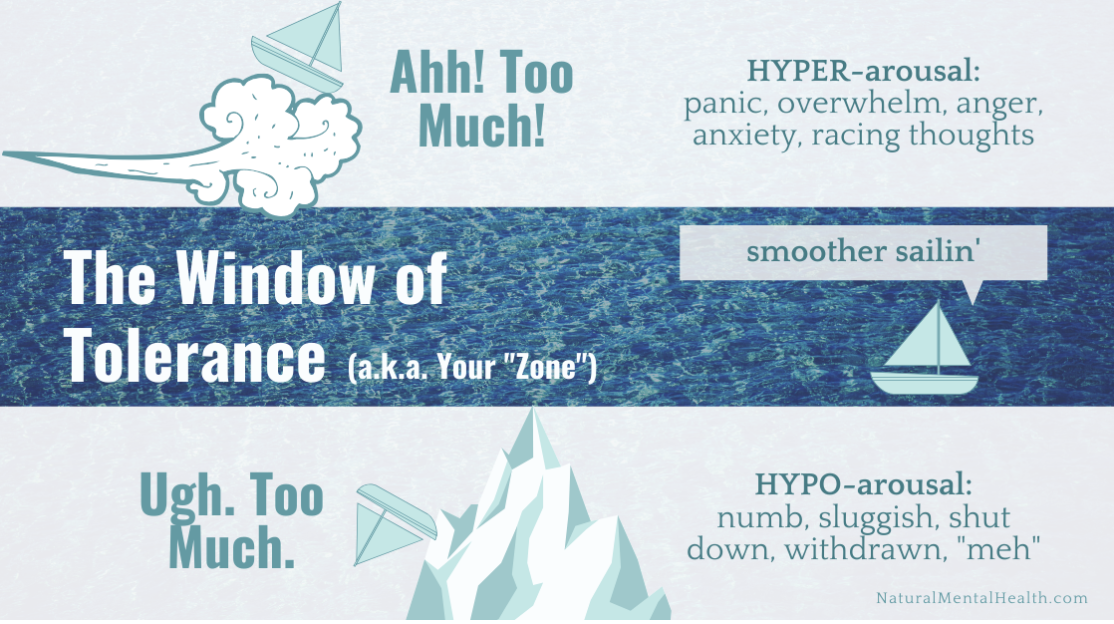
Applied to trauma, IPNB offers the idea of a window of tolerance. Inside the window, you can feel what you are feeling and still function. Above the window, you hit hyperarousal (chaos, overwhelm, panic). Below the window, you hit hypoarousal (collapse, numbness, shutdown). Trauma narrows the window. Healing widens it.
Crucially, IPNB also asserts that humans are self-healing systems. Given the right conditions, differentiation and linkage, relational safety, room to integrate experience, the body's natural push toward wholeness takes over. Your job in therapy is not to heal yourself by force of will. It is to cooperate with a process your system already knows how to run.
Emotion Theory: Your Feelings Are Not the Enemy
Finally, drawing on Karla McLaren's work, I hold a specific view of emotions that I think is essential to get right early. Emotions are not problems to eliminate. They are the body's language.
Anger arises when something valuable is threatened; its purpose is to protect and restore. Sadness arises when something valuable must be released; its purpose is to help us let go. Depression can be the body's way of slowing everything down so a person can finally pay attention to something that needs processing. Anxiety, rightly understood, is the body mobilizing energy and focus for something it considers important. Even states we typically treat as pathological are often communications the body is making in the language it has.
This matters because a common, unspoken hope survivors bring into healing work is: if I heal, I will never feel this bad again. I understand that hope. I have had it myself. But that is not what healing delivers, and promising it would be dishonest. What healing does offer is a new relationship with feelings: enough space to experience them without being overwhelmed by them, enough literacy to understand what they are saying, and enough trust in your own system to respond instead of react. The mechanism of feeling stays. The siege ends.
What Healing Trauma Does Not Mean
Let me be plain about a few things, because the field sometimes is not.
Healing is not the elimination of difficult feelings. You will still feel sad, angry, anxious, even terrified at times. Life produces those states in non-traumatized nervous systems too. What changes is your relationship to them and your capacity to move through them.
Healing is not a finish line. It is a process with meaningful milestones, not a destination you arrive at and hang a banner.
Healing is not one-size. What supports a survivor of a single adult event may look different from what supports a survivor of complex, early, repeated trauma. The right approach for you depends on your history, your nervous system, your relationships, and your spiritual orientation if you have one.
Healing cannot be promised on a timeline. Anyone who tells you "six weeks to recovery" is selling you something. Honest trauma work respects that the nervous system has its own pace, and that pace varies person to person.
What Healing Trauma Can Look Like in Practice
So what does healing actually produce? From my work with clients and from my own ongoing experience, some of what becomes possible includes:
A wider window of tolerance: more room to feel what is happening in the present without tipping into hyperarousal or shutdown.
Earned secure connection: relationships that feel safe, mutual, and sustaining, often for the first time.
Feelings as information, not sentences: a new ability to notice what your body is telling you and respond, instead of being hijacked by a reaction.
A recovered felt sense of safety in your own body: the deepest and, for many survivors, the most surprising gift of the work. Judith Blackstone describes this as the body becoming "unbound," no longer held in the defensive contractions that trauma carved into it (Blackstone, 2018). This outcome, the body returning to itself, shows up across the broader clinical literature on attachment-based and body-oriented trauma work (Solomon & Siegel, 2003).
These are not guarantees. They are possibilities that become more available the longer the work continues in the right conditions.
If you are wondering whether this kind of work could be right for you, the most useful next step is a conversation. My practice offers individual trauma recovery sessions, group-based work including The Octave for male survivors of sexual trauma, open-ended Complex-PTSD support groups, couples and family work, and workshops. I also offer trainings for healing professionals who want to bring body-based, integrative approaches into their own work.
Book a free consultation to explore what healing could mean for you specifically. You are not alone. You are not broken. And you can heal.
Frequently Asked Questions
-
Healing trauma means restoring your nervous system's capacity to feel safe, connected, and present, even though difficult feelings will still arise in life. It is a process of widening your window of tolerance, building secure relationships, and recovering a felt sense of safety in the body. It is not the elimination of all hard emotions, and it is not a single endpoint you arrive at.
-
There is no honest universal answer. Some survivors experience meaningful shifts within weeks of starting body-based work. Others, particularly those with Complex-PTSD or early repeated trauma, do the work over years. The pace depends on your history, your nervous system, your support system, and your access to consistent, attuned care. Anyone offering a guaranteed timeline is worth approaching with skepticism.
-
This depends on what "fully healed" means to you. If it means never feeling a trauma-related symptom again, that framing can set survivors up for disappointment. If it means no longer being ruled by the trauma, living with genuine connection and agency, and experiencing feelings without being overwhelmed by them, many survivors reach that place. My own experience and the experience of survivors I have worked with suggests that recovery is real and often goes further than people believed possible when they started.
-
Neither is universally better. Individual sessions offer depth, pacing, and privacy for material that needs a one-on-one container. Group work offers something individual work cannot replicate: the direct nervous system experience of not being alone with your story. Many survivors benefit most from a combination. The Octave, my group-based approach for male survivors of sexual trauma, exists because the peer-to-peer dimension turned out to be one of the most potent ingredients in healing, often before any formal technique was applied.
-
Complex-PTSD (C-PTSD) generally describes the constellation of symptoms that arise from prolonged, repeated trauma, often beginning in childhood and often occurring within relationships. It typically includes the symptoms of PTSD plus additional challenges around identity, emotion regulation, and relationships. Healing C-PTSD usually requires longer, more relational work than healing from a single adult event, and it often benefits from the co-regulation that group and attachment-based approaches offer.
-
You do not need to feel ready. Most survivors never quite do. What you need is a practitioner you feel minimally safe enough with to begin the conversation, and a willingness to move at a pace your nervous system can tolerate. A free consultation is a low-commitment way to test the waters. You are allowed to ask questions, to listen to how someone talks about the work, and to decide from there.
References
Aurobindo, Sri. (1990). The Synthesis of Yoga. Lotus Press.
Badenoch, B. (2018). The Heart of Trauma. W.W. Norton & Company.
Banerji, D. (2016). Seven Quartets of Becoming. Nalanda International.
Blackstone, J. (2018). Trauma and the Unbound Body. Sounds True.
Damasio, A. R. (2019). The Strange Order of Things: Life, Feeling, and the Making of Cultures. Vintage Books.
Herman, J. L. (2015). Trauma and Recovery. Basic Books.
Larson, G. J. (1969). Classical Samkhya. Motilal Banarsidass.
Levine, P. A., & Frederick, A. (1997). Waking the Tiger: Healing Trauma. North Atlantic Books.
Levine, P. A., & Kline, M. (2008). Trauma-Proofing Your Kids. North Atlantic Books.
McLaren, K. (2010). The Language of Emotions. Sounds True.
Miller, A. (1997). The Drama of the Gifted Child. Basic Books.
Porges, S. W. (2011). The Polyvagal Theory. W.W. Norton.
Porges, S. W. (2017). The Pocket Guide to Polyvagal Theory. W.W. Norton & Company.
Siegel, D. J. (2012). Pocket Guide to Interpersonal Neurobiology. W.W. Norton & Company.
Siegel, D. J. (2018). Aware: The Science and Practice of Presence. TarcherPerigee.
Solomon, M. F., & Siegel, D. J. (2003). Healing Trauma: Attachment, Mind, Body, and Brain. W.W. Norton.
Van der Kolk, B. A. (2015). The Body Keeps the Score. Penguin Books.